
Market Calm, but Change on the Horizon:
Miami, Florida
Community Report No. 08
Spring 1999
Colleen Hirshkorn, Sally Trude, Christina A. Andrews, Lawrence D. Brown
![]() n December 1998, a team of researchers visited Miami, Fla., to study that
community’s health system, how it is changing and the impact of those changes
on consumers. More than 70 leaders in the health care market were interviewed
as part of the Community Tracking Study by the Center for Studying Health
System Change (HSC) and The Lewin Group. Miami is one
of 12 communities tracked by HSC every two years through site visits
and surveys. Individual community reports are published for each round
of site visits. The first site visit, in December 1996, provided baseline
information against which changes
are being tracked. The Miami market encompasses Dade County.
n December 1998, a team of researchers visited Miami, Fla., to study that
community’s health system, how it is changing and the impact of those changes
on consumers. More than 70 leaders in the health care market were interviewed
as part of the Community Tracking Study by the Center for Studying Health
System Change (HSC) and The Lewin Group. Miami is one
of 12 communities tracked by HSC every two years through site visits
and surveys. Individual community reports are published for each round
of site visits. The first site visit, in December 1996, provided baseline
information against which changes
are being tracked. The Miami market encompasses Dade County.
![]() n 1996, the Miami-Dade
health care market was marked by extensive deal-making that created
expectations among local leaders that health plans and hospitals would
consolidate. Meanwhile, high Medicare payments and relatively attractive
Medicaid payment rates had lured many health plans to the market. Three
major hospital systems were engaged in aggressive
acquisition strategies, leaving the future of independent hospitals in
question. the expected roll-out of mandatory Medicaid managed care
raised concerns regarding the continued viability of safety net providers.
n 1996, the Miami-Dade
health care market was marked by extensive deal-making that created
expectations among local leaders that health plans and hospitals would
consolidate. Meanwhile, high Medicare payments and relatively attractive
Medicaid payment rates had lured many health plans to the market. Three
major hospital systems were engaged in aggressive
acquisition strategies, leaving the future of independent hospitals in
question. the expected roll-out of mandatory Medicaid managed care
raised concerns regarding the continued viability of safety net providers.
Since then, generous Medicare capitation rates have continued to fuel competition among the many health plans in this market. Although several hospital acquisitions have been finalized, there has been limited clinical consolidation or capacity reduction. Despite numerous efforts, few physician organizations have succeeded.
Among the key factors shaping the Miami-Dade health care market today:
- Hospital competition is easing, as hospitals solidify their positions.
- A variety of different physician organizations formed to assume financial risk, but many have struggled.
- Implementation of Medicaid managed care has proceeded without major disruption to the safety net.
Abundant Health Care Resources
![]() iami-Dade is a health care
market of abundance, with attractive payments from Medicare and Medicaid, and
an oversupply of providers and health plans. The market, a mix of urban,
suburban, ethnic and rural areas spanning more than 2,000 square miles,
is economically and culturally diverse, with Hispanics accounting for
approximately 50 percent of the population. The number of
hospital beds and physicians per capita are among the highest in the
12 communities tracked by HSC.
iami-Dade is a health care
market of abundance, with attractive payments from Medicare and Medicaid, and
an oversupply of providers and health plans. The market, a mix of urban,
suburban, ethnic and rural areas spanning more than 2,000 square miles,
is economically and culturally diverse, with Hispanics accounting for
approximately 50 percent of the population. The number of
hospital beds and physicians per capita are among the highest in the
12 communities tracked by HSC.
This wealth of resources contrasts with the poverty and lack of health insurance in some of Miami-Dade’s communities. One in four persons is uninsured, and the proportion of employers offering coverage is the lowest among the sites HSC tracks.
Public sector payment sources have had a dramatic impact on this market. The Medicare capitation rate ($763.19) is one of the highest in the country and has attracted many health plans. Despite exits from Medicare markets in other Florida counties where the rate is lower, health plans continue to compete for Medicare business in Dade, offering enrollees unlimited pharmacy benefits, zero premiums and no copayments. The Medicare 50/50 rule, which required all health plans participating in Medicare to have at least half of their enrollees in commercial plans, led to cross-subsidization of commercial rates, keeping them artificially low. With elimination of this rule in 1999, purchasers anticipate increases in commercial premiums. Furthermore, the Balanced Budget Act of 1997 is expected to moderate the flow of Medicare funds to plans and providers in the Miami-Dade market.
Medicaid also remains appealing to health plans, with relatively favorable reimbursement at 92 percent of fee-for-service rates. In addition, public monies from a half-cent sales tax in Dade County support care for the uninsured via the area’s public hospital, Jackson Memorial Hospital (JMH), and its affiliated clinics.
Neither public nor private employers have had significant influence on the health care market, other than through price-conscious purchasing. The state’s Community Health Purchasing Alliance (CHPA) program was launched in 1993 to help small businesses-a large component of Miami-Dade’s private employer sector-offer health insurance to their employees. However, this program has not attracted large numbers of businesses. The Miami CHPA, with 3,550 member firms, reports that this failure is due to its inability to contract selectively with health plans, meaning it must take whatever price plans offer. One of the market’s largest employers is the county school system, but even its influence is limited. Its recent attempt to drop one health plan due to poor performance was reportedly reversed due to political pressures.
On the heels of health plan fraud and abuse scandals in the 1980s, the Florida state legislature in 1992 mandated national accreditation for all health plans, and the state was an early adopter of an external appeals policy. Florida also has recently strengthened consumer protection legislation and mandated a report card on health plan performance. Because broad provider networks ensure consumer choice, purchasers are less concerned about medical quality and related report cards than they are about resolving customer service problems. Purchasers said that poor customer service is their top concern.
Hospital Competition Subsides
![]() n 1996, the
Miami-Dade hospital market was characterized by intense competition.
The three principal hospital systems - Baptist Health Systems,
Columbia/HCA and Tenet Healthcare Corp. - were actively acquiring
other hospitals to increase their market share and lower costs.
Baptist Health was discussing a merger with Mercy Hospital to
solidify its position in south Dade and expand service to the
Hispanic community. Both Columbia/ HCA and Tenet were eyeing new
acquisitions and affiliations to address gaps in service and market coverage. The future of the remaining independent hospitals was unclear.
Several of them were considering mergers or other formal relationships
with the three major systems.
n 1996, the
Miami-Dade hospital market was characterized by intense competition.
The three principal hospital systems - Baptist Health Systems,
Columbia/HCA and Tenet Healthcare Corp. - were actively acquiring
other hospitals to increase their market share and lower costs.
Baptist Health was discussing a merger with Mercy Hospital to
solidify its position in south Dade and expand service to the
Hispanic community. Both Columbia/ HCA and Tenet were eyeing new
acquisitions and affiliations to address gaps in service and market coverage. The future of the remaining independent hospitals was unclear.
Several of them were considering mergers or other formal relationships
with the three major systems.
Over the past two years, however, the high level of competition anticipated among hospital systems has subsided. Two factors appear to account for this phenomenon. First, the perceived threat of Columbia/HCA to local not-for-profit hospitals dissipated, largely because its attention was diverted by an ongoing federal investigation. Second, hospitals have continued to pursue geographically and demographically based strategies to solidify their market niches, allowing them to carve out distinct submarkets and thus minimize direct competition. Tenet expanded its presence in north Dade through its national merger with OrNda and its acquisition of Hialeah Hospital and North Shore Medical Center, and it is now expanding north into Broward and Palm Beach counties. In south Dade, Baptist Health remains the dominant provider, with its ownership of Baptist, South Miami and Homestead hospitals. Baptist also attempted to expand its market share in south Dade through a merger with Mercy Hospital, a Catholic facility, but the merger failed due to differences over reproductive health and end-of-life decisions.
Free-standing hospitals have also solidified their market positions. Mount Sinai Medical Center’s distinct geographic service area in Miami Beach has ensured its inclusion in most health plan networks. Pan American Hospital maintained its independence by strengthening its ties with the Hispanic community; it is operating at full occupancy and is profitable. The independent status of these hospitals now seems stronger.
At the same time, JMH, a tertiary care facility, appears to have strengthened its position. The hospital is planning an affiliation with Columbia/HCA’s Deering Hospital to increase its presence in south Dade. It is also expanding its primary care capacity by opening a primary care center two miles from the hospital campus and by contracting with primary care physicians in the suburbs. Together, these activities are expected to help JMH build its commercial and Medicaid business, increasing its paying patient base and its provision of more routine procedures, such as uncomplicated births.
In a related move, the JMH-sponsored health plan recently won the sole contract in Miami-Dade to cover enrollees in the state’s Child Health Insurance Program (CHIP), KidCare. The expectation is that this contract will strengthen JMH’s financial position as well by bringing additional revenue and referrals to the hospital.
While most of Miami-Dade’s hospital market appears to be in a period of stability, JMH’s expansion activities may disrupt this equilibrium. As JMH continues to pursue a more geographically decentralized approach and a broader patient base, the impact on Miami-Dade’s hospital market remains to be seen.
Physician Organizations Develop, but Few Succeed
![]() n 1996, most
Miami-Dade physicians practiced in small single-specialty groups.
The only long-standing physician organization in the market is the
University of Miami Medical Group,
a faculty practice plan with more than 600 academic physicians
affiliated with JMH and Miami Children’s hospitals. Hospitals
were beginning to develop physician-hospital organizations (PHOs)
and independent practice associations (IPAs) as vehicles to assume risk.
n 1996, most
Miami-Dade physicians practiced in small single-specialty groups.
The only long-standing physician organization in the market is the
University of Miami Medical Group,
a faculty practice plan with more than 600 academic physicians
affiliated with JMH and Miami Children’s hospitals. Hospitals
were beginning to develop physician-hospital organizations (PHOs)
and independent practice associations (IPAs) as vehicles to assume risk.
Meanwhile, the oversupply of physicians in Miami-Dade spurred national management companies and physician entrepreneurs to develop physician organizations. Most of these organizations, however, have been largely unsuccessful. Lack of information infrastructure, problematic reimbursement strategies and reluctance by health plans to share risk have thwarted these efforts, and many have proven to be short-lived.
National physician practice management companies (PPMCs), such as PhyCor, MedPartners and FPA, came to Miami-Dade over the past two years. But consistent with their experience nationally, these firms struggled in vain to meet physicians’ financial expectations and their own bottom lines. Some have left Miami-Dade. Other companies, such as VIVRA, managed specialty networks for health plans. These ventures not only experienced financial difficulties, but also disrupted plan-provider relationships.
Hospitals, meanwhile, continued to develop and support several large PHOs and IPAs to increase their leverage with health plans and protect referrals. But this strategy won them few risk-based contracts, and hospitals and physicians alike seem disenchanted with these organizations. The Tenet hospitals are planning to abandon some of their PHOs and to reorganize their physicians into an IPA, but the implications of this change are unclear. DadeWell, a 600-member IPA formed by Baptist Health in 1996, has struggled to obtain globally capitated contracts, and it has not generated as much referral volume as physicians anticipated.
Frustrated by the bureaucracy of national management companies and the inadequacies of the hospital-sponsored organizations, some local physicians have begun their own organizational efforts. FemWell is one example. Its 60 physicians, who together represent about 80 percent of the obstetrics and gynecology business of Mercy, Baptist and South Miami hospitals, have banded together to contract with health plans. With just a 2 percent management fee, FemWell has reportedly begun to increase physician practice revenues and improve its position relative to health plans in the market. PhyTrust is another new entity, which manages globally capitated contracts with HMOs for participating primary care physicians.
While the future of FemWell and PhyTrust remains to be seen, physician organizations on the whole have struggled in Miami-Dade. It is unclear whether an effective organizational model will take hold in this market and what the relative roles of physicians, hospitals, health plans and national management companies in such a model might be.
Medicaid Managed Care Proceeds without Competitive Bidding
![]() wo years ago, the prospect
of Medicaid managed care worried providers and health plans alike. Safety net
providers feared declines in their Medicaid
revenues, as recipients were shifted
from traditional fee-for-service arrangements to managed care options that might
redirect patients to other providers (and therefore redistribute Medicaid funds).
Health plans fought the state’s attempt to establish enrollment levels based on
quality measures, and blocked the state’s plan for competitive Medicaid contract
bidding.
wo years ago, the prospect
of Medicaid managed care worried providers and health plans alike. Safety net
providers feared declines in their Medicaid
revenues, as recipients were shifted
from traditional fee-for-service arrangements to managed care options that might
redirect patients to other providers (and therefore redistribute Medicaid funds).
Health plans fought the state’s attempt to establish enrollment levels based on
quality measures, and blocked the state’s plan for competitive Medicaid contract
bidding.
The state now contracts with any HMO willing to accept 92 percent of the fee-for-service rate and meet certain quality requirements. For example, Medicaid plans in Florida must be licensed and nationally accredited, like commercial and Medicare plans. Having previously backed away from applying these quality standards to Medicaid plans, the state recently reinstated them. In addition, plans contracting with Medicaid are required to provide certain preventive health services, such as prenatal care and domestic violence services, which go beyond the scope of the basic Medicaid benefit package.
Nine HMOs in the Miami-Dade market were awarded contracts when the state began mandatory Medicaid managed care enrollment in 1997. Since then, Medicaid managed care has proceeded without much contention. Plans expressed little reaction to the decrease in reimbursement rates from 95 to 92 percent of fee-for-service rates; no plan has exited the Medicaid program.
However, health plan respondents expressed frustration about their administrative burden under the program.
- Discontinuity of enrollment appears to be the major concern for health plans.
The high turnover in Medicaid eligibility and frequent plan switching make this
a very unstable population for health plans, and the state legislature is
considering a six-month lock-in policy to address this issue.
- Respondents also said that the state’s decision to outsource Medicaid
enrollment functions to an independent contractor has caused some confusion.
- Health plan respondents noted the difficulty of managing the auto-assignment
process and meeting the program’s reporting requirements along with
other state and federal mandates.
- Finally, in the absence of competitive bidding, plans have no guarantee of enrollment numbers. This uncertainty, coupled with restrictions on direct marketing, has left some plans with limited ability to manage this business.
Safety net providers faced a potential setback with the renewed requirement that plans serving the Medicaid population be commercially licensed and nationally accredited. This threatened the continued participation of safety net provider-sponsored plans that did not have the reserves or infrastructure to meet these standards. In response, a network of community health centers (CHCs), Health Choice Network, pursued an alternate strategy to secure and shore up Medicaid revenue. The CHCs formed a management service organization (MSO), Atlantic Care, to help manage the CHCs’ Medicaid managed care business. Atlantic Care holds a full risk contract with the HMO, Physicians Healthcare Plans, for its Medicaid enrollees. Atlantic Care reportedly is up and running, with steadily increasing enrollment and a substantial return on the CHCs’ initial investment.
In addition, under a special state pilot project, JMH has partnered with the North and South Broward Hospital Districts to enroll Medicaid beneficiaries in a new health plan with a more limited network that emphasizes more traditional safety net providers. The health plan is expected to begin operating this spring.
Safety Net Appears Relatively Stable
![]() mplementation of Medicaid
managed care does not appear to have undermined Miami-Dade’s safety net providers,
as some feared it would. There were
scattered reports of some CHC service reductions as a result of declining
Medicaid reimbursement; however,
many safety net providers are working cooperatively to meet Miami-Dade’s
staggering burden of indigent care.
mplementation of Medicaid
managed care does not appear to have undermined Miami-Dade’s safety net providers,
as some feared it would. There were
scattered reports of some CHC service reductions as a result of declining
Medicaid reimbursement; however,
many safety net providers are working cooperatively to meet Miami-Dade’s
staggering burden of indigent care.
Because of its role under the Public Health Trust, JMH has been central to many of these efforts. JMH and its affiliated centers were designated as the sole recipients of the county’s Public Health Trust funds for indigent care when the trust was established with the half-cent sales tax passed in 1991 and other local, state and federal funds. Although JMH’s designation has been the subject of some controversy, the hospital appears to have lessened opposition to its continued hold on this revenue by affiliating with other safety net providers, including the Community Health Initiative of South Dade (CHI). JMH will provide CHI both technical assistance in financial management and short-term monetary support.
Partnership discussions are also reportedly underway between the Public Health Trust and Homestead Hospital in south Dade, which provides a significant level of uncompensated care. There is particular concern about indigent care needs in south Dade, where poverty and uninsurance rates are very high and rising and where, until recently, JMH has not had any facilities.
Meanwhile, several efforts are underway to respond to concerns about indigent care through a more community-based approach. For example, the Dade County Public Health Authority recently contracted with the South Florida Health Council to develop information on the health care needs of south Dade’s indigent population and strategies to address them. In addition, Camillus Health Concern, a CHC for the homeless, is seeking partnerships with the Public Health Trust and other local entities to improve the health of the underserved in Miami-Dade.
At the state level, there have also been recent expansions to children’s health insurance options, through a program known as KidCare. With funding from the federal CHIP, the Florida legislature broadened Medicaid eligibility for children and expanded the state-subsidized health insurance program, Florida Healthy Kids. KidCare is expected to cover an estimated 35,000 additional children in the Miami-Dade area.
Optimism about the expanded insurance coverage for children has been tempered by concerns about outreach and enrollment, especially for immigrant children. Even if the program reaches its enrollment targets, it will only begin to make a dent in the problem in Miami-Dade, where, according to HSC data, roughly 100,000 children - or one in five of all children - are uninsured.
Issues to Track
![]() he Miami-Dade health
care market appears to have entered a period of relative calm. Competition
among hospitals has diminished as these providers solidify their market
positions and the threat of continued acquisitions has receded. Health
plans continue to be sustained by lucrative Medicare payments that, until
recently, have cross-subsidized commercial premiums. Physician organizations
have met with little success, causing some turmoil in the market, but producing
no major change in the organization or financing of care to date. While
persistent poverty and lack of health insurance remain significant problems,
safety net providers appear stable.
he Miami-Dade health
care market appears to have entered a period of relative calm. Competition
among hospitals has diminished as these providers solidify their market
positions and the threat of continued acquisitions has receded. Health
plans continue to be sustained by lucrative Medicare payments that, until
recently, have cross-subsidized commercial premiums. Physician organizations
have met with little success, causing some turmoil in the market, but producing
no major change in the organization or financing of care to date. While
persistent poverty and lack of health insurance remain significant problems,
safety net providers appear stable.
Against this backdrop, there are a number of key issues to track:
- What impact will the elimination of
the Medicare 50/50 rule and slowed growth in Medicare payments have
on the market? How will commercial premiums be affected by these changes, and
how will employers respond?
- What impact will Jackson Memorial’s expansion have on the nature of
competition among Miami-Dade hospitals? How will these efforts affect its
position as an indigent care provider?
- Will an effective organizational model emerge that allows physicians to
gain leverage in the Miami-Dade market?
- How will the community and state and local policy makers address the heavy health care burdens created by poverty and lack of health insurance?
Miami Compared to Other Communities HSC Tracks
Miami, the highest and lowest HSC study sites and metropolitan areas with over 200,000 population
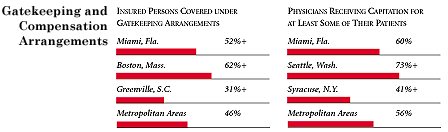
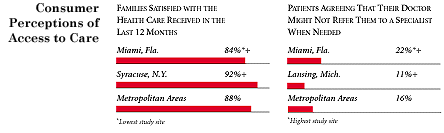


+ Site value is significantly different from the mean for metropolitan
areas over 200,000 population.
The information in these graphs comes from the Household, Physician and Employer
Surveys conducted in 1996 and 1997 as part of HSC’s Community Tracking Study. The
margins of error depend on the community and survey question and include +/- 2
percent to +/- 5 percent for the Household Survey, +/-3 percent to +/-9 percent
for the Physician Survey and +/-4 percent to +/-8 percent for the Employer Survey.
Background and Observations
Miami Demographics
| Miami, Fla. | Metropolitan areas above 200,000 population |
| Population, 19971 | |
| 2,044,600 | |
| Population Change, 1990-19971 | |
| 5.3% | 6.7% |
| Median Income2 | |
| $19,811 | $26,646 |
| Persons Living in Poverty2 | |
| 22% | 15% |
| Persons Age 65 or Older2 | |
| 15% | 12% |
| Persons with No Health Insurance2 | |
| 24% | 14% |
|
Sources: 1. U.S. Census, 1997 2. Household Survey Community Tracking Study, 1996-1997 | |

The Community Tracking Study, the major effort of HSC, tracks changes in the health system in 60 sites that are representative of the nation. Every two years, HSC conducts surveys in all 60 communities and site visits in the following 12 communities:
- Boston, Mass.
- Cleveland, Ohio
- Greenville, S.C.
- Indianapolis, Ind.
- Lansing, Mich.
- Little Rock, Ark.
- Miami, Fla.
- Newark, N.J.
- Orange County, Calif.
- Phoenix, Ariz.
- Seattle, Wash.
- Syracuse, N.Y.