
Ownership Changes Set Market in Flux:
Phoenix, Arizona
Community Report No. 09
Spring 1999
Jon B. Christianson, Cara S. Lesser, Caroline Rossi Steinberg, June Eichner
![]() n December 1998, a team of researchers visited Phoenix, Ariz., to study that
community’s health system, how it is changing and the impact of those changes on
consumers. More than 40 leaders in the health care market were interviewed as part
of the Community Tracking Study by the Center for Studying Health System Change
(HSC) and The Lewin Group. Phoenix is one
of 12 communities tracked by HSC every two years through site visits and surveys.
Individual community reports are published for each round of site
visits. The first site visit to Phoenix,
in December 1996, provided baseline information against which changes are being
tracked. The Phoenix market includes Maricopa and Pinal counties.
n December 1998, a team of researchers visited Phoenix, Ariz., to study that
community’s health system, how it is changing and the impact of those changes on
consumers. More than 40 leaders in the health care market were interviewed as part
of the Community Tracking Study by the Center for Studying Health System Change
(HSC) and The Lewin Group. Phoenix is one
of 12 communities tracked by HSC every two years through site visits and surveys.
Individual community reports are published for each round of site
visits. The first site visit to Phoenix,
in December 1996, provided baseline information against which changes are being
tracked. The Phoenix market includes Maricopa and Pinal counties.
![]() hoenix has experienced some of the
fastest population growth in the country, attracting the entry
of health plans, the creation of new facilities and
the development of geographic submarkets for health care. In 1996, several potential
changes faced the Phoenix market: two of the major hospital systems considered but
rejected a merger, the area’s public health care system was in a financial crisis,
physicians began to consolidate and national for-profit health plans became
increasingly dominant.
hoenix has experienced some of the
fastest population growth in the country, attracting the entry
of health plans, the creation of new facilities and
the development of geographic submarkets for health care. In 1996, several potential
changes faced the Phoenix market: two of the major hospital systems considered but
rejected a merger, the area’s public health care system was in a financial crisis,
physicians began to consolidate and national for-profit health plans became
increasingly dominant.
Since then, major changes in the hospital sector have emerged, as the two systems that considered a merger established other strategic affiliations. For-profit health plans have solidified their position, and although the public system has weathered its financial crisis, its future is uncertain. Other developments include:
- The market’s largest not-for-profit provider system has been dramatically reconfigured.
- National physician practice management companies (PPMCs) failed locally, but physicians are seeking other organizational and entrepreneurial opportunities.
- New funding sources for the uninsured have emerged.
- Large Provider System Reconfigures, Hospital Market in Flux
- Health Plan Market in Transition
- Physicians Regroup as PPMCs Fail, Specialists Consolidate
- Hospitals and Physicians Struggle with New Relationships
- Tobacco Tax Provides Support for Indigent Care
- County Health System Stabilizes Financially but Remains in Flux
- Issues to Track
- Phoenix Compared to Other Communities HSC Tracks
- Background and Observations
Large Provider System Reconfigures, Hospital Market in Flux
![]() ocally based Samaritan Health
System, the state’s largest health care system, has undergone dramatic changes
during the past two years, in the aftermath of a failed merger attempt with
Mercy Healthcare Arizona, owned by Catholic Healthcare West (CHW). Samaritan’s
reconfiguration holds potentially major implications for other local health care
systems, competition in the health plan market and the future of the state’s
prepaid Medicaid program, the Arizona Health Care Cost Containment System (AHCCCS).
ocally based Samaritan Health
System, the state’s largest health care system, has undergone dramatic changes
during the past two years, in the aftermath of a failed merger attempt with
Mercy Healthcare Arizona, owned by Catholic Healthcare West (CHW). Samaritan’s
reconfiguration holds potentially major implications for other local health care
systems, competition in the health plan market and the future of the state’s
prepaid Medicaid program, the Arizona Health Care Cost Containment System (AHCCCS).
In 1996, Samaritan was Phoenix’s largest system, with hospitals located throughout the metropolitan area. In addition to its 582-bed Good Samaritan Regional Medical Center in central Phoenix, it owned three hospitals in suburban areas, two rural hospitals and two skilled nursing facilities. It also owned Arizona Physicians IPA, the largest health plan contracting with AHCCCS, and cosponsored HealthPartners Health Plans, the only commercial health plan owned by local providers.
After merger discussions with Mercy foundered in 1997, Samaritan tried to solve its financial problems by solidifying its position in Phoenix’s acute care market. Samaritan decided to divest itself of several components it did not consider essential to this strategy. First, it sold Maryvale Samaritan Medical Center to Vanguard Health System, a Nashville-based, for-profit chain, and its two rural hospitals to other buyers. At the same time, Samaritan expressed interest in acquiring financially troubled Chandler Regional Hospital in the rapidly growing East Valley and shoring up its own pediatric capacity at its downtown hospital.
In a second major move, Samaritan sold both of its health plans to United Healthcare, a national for-profit company. Then, in 1998, Samaritan announced its intent to be acquired by Lutheran Health System, a not-for-profit hospital chain based in Fargo, N.D., which at the time owned two hospitals in southeast Phoenix.
If the Samaritan-Lutheran deal proceeds, a national hospital system will, for the first time, become the dominant provider of inpatient services in Phoenix. The announcement of this merger has already had several significant effects and promises further changes:
- First, Samaritan withdrew its bid for Chandler Hospital, leaving the field
open to competitors. CHW ultimately acquired Chandler, marking the first time
it successfully affiliated with another hospital in Phoenix. Moreover, the
affiliation gave CHW a foothold in
the rapidly growing East Valley, where
it could compete with the merged Samaritan-Lutheran system.
- Second, with the sale of HealthPartners to United Healthcare, other health
systems are eyeing HealthPartners’ 218,000 members as potential new business
and are positioning to negotiate with United. If they succeed, Samaritan stands to
lose some patients to other hospitals.
- Third, respondents speculated that United’s acquisition of Arizona Physicians IPA could have a negative impact on AHCCCS.
Other hospital-based systems in central Phoenix are struggling to maintain market share, while those in the suburbs generally remain strong. Tenet Healthcare Corp., which owns four hospitals in the area, recently announced plans to pull out of Phoenix in keeping with a national decision to exit areas where it has not gained substantial market share. At the same time, Phoenix Children’s Hospital, which currently leases space on the Samaritan downtown campus and contracts with the hospital system for certain services, is considering affiliating with CHW or pursuing a more independent approach. The county hospital system, Maricopa Integrated Health System, is also considering a major reconfiguration. In addition, the Mayo Clinic recently opened a newly constructed hospital in Scottsdale.
Collectively, the changes indicate continued upheaval in the Phoenix hospital market and suggest an emerging emphasis on suburban submarkets.
Health Plan Market in Transition
![]() he dynamics of Phoenix’s highly
competitive health plan market are changing significantly in all sectors. In
Medicare, new financial concerns stemming from anticipated slow growth in
payment rates, along with the prospect of competitive bidding, are likely
to intensify competition among Medicare risk plans. Meanwhile, the role
of commercial plans in
the AHCCCS program is in flux, and
the privately insured market has become almost entirely the province of
for-profit national plans.
he dynamics of Phoenix’s highly
competitive health plan market are changing significantly in all sectors. In
Medicare, new financial concerns stemming from anticipated slow growth in
payment rates, along with the prospect of competitive bidding, are likely
to intensify competition among Medicare risk plans. Meanwhile, the role
of commercial plans in
the AHCCCS program is in flux, and
the privately insured market has become almost entirely the province of
for-profit national plans.
Medicare. In 1996, the Medicare market was hotly contested, with competition focused primarily on benefits and provider choice, given high payment rates. Medicare health maintenance organization (HMO) enrollees typically paid no premiums and enjoyed extensive benefits, such as health club memberships. A high level of competition continues, even though Medicare payment rates have increased by only about 5 percent during the past two years.
Two emerging issues are likely to dramatically reshape Medicare managed care in Phoenix:
- Medicare payment to Phoenix health plans is expected to decline in the coming
years, due to relatively small rate increases and implementation of risk adjustment
established by the Balanced Budget Act
of 1997. As a result, some respondents predicted that plans may scale back their
benefits, particularly for prescription drugs, and institute premiums.
- Phoenix is a test site for a new competitive bidding approach to setting Medicare reimbursement rates for contracting health plans. If plans bid below the average rate set for a standard benefit package, they keep the difference in profit or can use it to add benefits to the standard package; plans bidding above the average rate will have to charge beneficiaries a premium. If implemented, this strategy could fundamentally change health plan competition for Medicare enrollees in Phoenix. However, there is local opposition to the project, and delays are already anticipated.
Medicaid. Commercial health plan participation in AHCCCS has shifted over the past two years, with two major plans leaving the market and one new plan entering. In 1996, some respondents speculated that several commercial plans had entered the AHCCCS market by submitting low bids and might not be able to continue to participate at such low reimbursement rates. By 1997, Blue Cross and Blue Shield of Arizona and Intergroup, an HMO owned by a national, for-profit company, dropped out of AHCCCS. United Healthcare’s entry into the Medicaid market through its purchase of Arizona Physicians IPA is an even more significant development. Arizona Physicians IPA has the largest number of AHCCCS enrollees in Phoenix and has won several awards for its innovative programming. Although United has said it will continue to participate in AHCCCS, respondents expressed concern that it will not honor this commitment if its AHCCCS contract is not profitable.
Commercial. Phoenix’s privately insured market essentially has been taken over by national, for-profit health plans; the only remaining local plan is Blue Cross and Blue Shield. By purchasing HealthPartners, the other locally owned plan, United Healthcare, leads the commercial HMO market. PacifiCare Health Systems, Inc., also increased its stake in the Phoenix market with its purchase of FHP International Corp. The Mayo Clinic, which launched its Mayo Health Plan in 1998 to compete in the commercial market only, plans to build enrollment gradually and is not expected to become a major player.
Physicians Regroup as PPMCs Fail, Specialists Consolidate
![]() n 1996, two trends suggested
an increasing level of physician consolidation in Phoenix: the acquisition of
primary care practices and multispecialty groups by PPMCs and the development
of locally based, single-specialty physician networks to contract with managed
care plans. Since 1996, PPMCs have failed locally, but the growth of
single-specialty networks has continued at a modest pace.
n 1996, two trends suggested
an increasing level of physician consolidation in Phoenix: the acquisition of
primary care practices and multispecialty groups by PPMCs and the development
of locally based, single-specialty physician networks to contract with managed
care plans. Since 1996, PPMCs have failed locally, but the growth of
single-specialty networks has continued at a modest pace.
The financial difficulties that have plagued for-profit PPMCs nationally have been evident in Phoenix. For example, when for-profit FPA Medical Management, Inc., purchased the long-established, Phoenix- and Tucson-based multispecialty group Thomas Davis Medical Centers in 1997, it instituted several cost-saving measures. Physicians resisted these changes, and many doctors left. FPA declared bankruptcy in July 1998, and Thomas Davis subsequently dissolved. About one-quarter of the Thomas Davis physicians in Phoenix who had not departed previously left the state, and the rest formed single-specialty groups, started their own practices or affiliated with existing practices. MedPartners has disposed of its physician practices in Phoenix, while PhyCor, Inc., sold its Arizona Physicians Center to Columbia/HCA. Although the departure of these firms affects only a small proportion of Phoenix physicians, the failure of PPMCs has made primary care physicians less willing to assume risk in contractual arrangements with health plans.
Affecting a far larger number of physicians, single-specialty networks continue to grow, though gradually. These networks, most of which are locally owned and managed, provide a vehicle for specialists to secure capitated contracts with managed care organizations. Networks of cardiologists, general surgeons, orthopedic surgeons and oncologists are contracting with several health plans in Phoenix. In a relatively new development, five groups of hospitalists - physicians who specialize in managing inpatient care - have formed, and increasing numbers of health plans are contracting with them.
Taken together, these developments suggest that the consolidation of Phoenix physicians - as in other communities - has taken on more of a single-specialty focus, moving away from the primary care and multispecialty approach that once appeared to be growing more rapidly.
Hospitals and Physicians Struggle with New Relationships
![]() ospital-based health systems in
Phoenix have had mixed results in their use of
physician-hospital organizations (PHOs)
to partner with physicians and increase their leverage with managed care plans.
This strategy has proved most successful
for systems in suburban areas that serve geographically limited markets and have
greater contracting clout with health plans. Other PHOs have not fared so well.
One started by St. Joseph’s Hospital, CHW’s flagship facility in Phoenix, folded
after losing about $3.5 million in only two years of operation. Two other PHOs
also shut down.
ospital-based health systems in
Phoenix have had mixed results in their use of
physician-hospital organizations (PHOs)
to partner with physicians and increase their leverage with managed care plans.
This strategy has proved most successful
for systems in suburban areas that serve geographically limited markets and have
greater contracting clout with health plans. Other PHOs have not fared so well.
One started by St. Joseph’s Hospital, CHW’s flagship facility in Phoenix, folded
after losing about $3.5 million in only two years of operation. Two other PHOs
also shut down.
Respondents offered several possible reasons why these PHOs have had difficulty succeeding. First, many health plans have resisted contracting with PHOs, preferring to negotiate directly with physicians. Second, some respondents said that PHOs, which typically are led by hospital administrators, have failed to garner the trust of physicians. As a result, physicians view PHOs as negotiating good deals for hospitals but not for them. Finally, physician respondents note PHOs’ high management fees as another factor contributing to their difficulties.
In light of these failures, some physicians are exploring other opportunities with hospitals - and independent of them - to shore up their practices and declining incomes. For physicians not in capitated arrangements, reimbursement is based on discounted Medicare rates, which have been stable at best or decreasing, especially for procedurally based specialists. In hopes of increasing income, some specialty groups are seeking joint ventures with hospitals and other entities. For example, three cardiologists have an equity partnership in the Arizona Heart Hospital, a new, for-profit facility with financial backing from North Carolina-based MedCath. Other specialists are pressuring local hospitals to build dedicated facilities and provide physicians with an equity share in these ventures and a significant decision-making role.
Some hospitals are responding, partly out of fear that if they do not, their physicians will defect. For example, Lutheran agreed to a joint venture with its cardiologists after MedCath approached the cardiologists with a proposal to jointly develop a free-standing heart hospital in the southeast suburbs.
Phoenix’s hospital systems are struggling with the demands of their specialist physicians to develop and expand partnership opportunities. Hospitals do not want to cede revenues to physicians, yet they recognize their dependence on specialists for admissions. Many hospitals are attempting to expand traditional programs that favor specialists but do not require physician investment or risk taking - for example, by building outpatient facilities with favorable lease arrangements for physicians. Respondents noted that these types of activities have heightened competition among health care systems in specialty service lines.
Tobacco Tax Provides Support for Indigent Care
![]() hoenix has an important new source
of funding for the uninsured. Under a 1994 ballot initiative, a tobacco tax was
approved, with 70 percent of revenues targeted for indigent health care. Annual
revenue from the tax has ranged from $125 million to $160 million. The tobacco
tax revenue first became available in 1996, and $34 million was appropriated to
indigent care. Additional revenue has since been allocated as the state’s matching
portion of Arizona’s Children’s Health Insurance Program, KidsCare, which began
enrollment in November 1998.
hoenix has an important new source
of funding for the uninsured. Under a 1994 ballot initiative, a tobacco tax was
approved, with 70 percent of revenues targeted for indigent health care. Annual
revenue from the tax has ranged from $125 million to $160 million. The tobacco
tax revenue first became available in 1996, and $34 million was appropriated to
indigent care. Additional revenue has since been allocated as the state’s matching
portion of Arizona’s Children’s Health Insurance Program, KidsCare, which began
enrollment in November 1998.
Tobacco tax funds have been used to develop new primary care clinics, increase staff and services at existing health centers, subsidize care for medically needy patients with end-stage renal disease and develop a premium-sharing program for the working poor who are not eligible for AHCCCS. This source of revenue is particularly important because it is the only source of funds in the state to provide care for undocumented immigrants.
The uninsured population in Phoenix appears to be growing. In 1996, HSC found that 16 percent of people in the Phoenix metropolitan statistical area were uninsured; two recent local surveys reported that the proportion of uninsured was 25 to 27 percent. Even though the number of jobs in Phoenix has increased steadily, many of the new positions are in the service industries, where employer-sponsored health insurance often is not offered. Also, the decoupling of Medicaid and cash assistance under welfare reform reportedly has contributed to the growth of Phoenix’s uninsured population.
County Health System Stabilizes Financially but Remains in Flux
![]() aricopa Integrated Health System
is Phoenix’s dominant safety net provider, serving AHCCCS enrollees and the
uninsured. In a financial crisis two years ago, the system has stabilized under
management by an outside contractor, but its future remains uncertain. Facing
severe financial losses, the County Board of Supervisors entered into a management
contract in 1997 with Quorum Health Group, Inc., a for-profit hospital management
company. Quorum’s contract was later extended through June 1999.
aricopa Integrated Health System
is Phoenix’s dominant safety net provider, serving AHCCCS enrollees and the
uninsured. In a financial crisis two years ago, the system has stabilized under
management by an outside contractor, but its future remains uncertain. Facing
severe financial losses, the County Board of Supervisors entered into a management
contract in 1997 with Quorum Health Group, Inc., a for-profit hospital management
company. Quorum’s contract was later extended through June 1999.
Under Quorum’s management, the system is now profitable on a month-to-month basis, although the hospital facility continues to suffer from lack of capital investment. The reasons for this reversal are a matter of debate in Phoenix. Quorum contends that it has reorganized operational systems, negotiated more favorable contracts with physicians, developed new service lines and used the new tobacco tax funds to increase services to the uninsured. Skeptics paint a somewhat different picture. Some argue that the system’s problems were not as severe as they initially appeared. Others say that Quorum has cut staff and programs substantially and instituted new and more burdensome cost-sharing requirements for the uninsured.
Even as the county health system stabilizes, a major reconfiguration is under consideration. The state plans to move to a competitive bidding process for the Arizona Long Term Care System (ALTCS), the long-term care equivalent of AHCCCS. Maricopa Integrated Health System has been the county’s sole contractor for ALTCS; with this change, it expects to lose substantial revenue. In light of this and other challenges, the county is exploring several possibilities for the health system, including sale, affiliation, partnership with a local entity, extension of Quorum’s management contract or negotiation of a new management contract with another entity.
This continued uncertainty surrounding the county system is a significant concern in Phoenix. Other health care systems fear they may be asked to increase the share of care they provide to the uninsured, while several respondents expressed concern that these changes may leave the poor and the growing uninsured population with more restricted access to care.
Issues to Track
![]() uring the past two years, national
for-profit managed care companies have solidified their hold on Phoenix’s health
plan market. The largest local hospital system has undergone dramatic
reconfiguration and has aligned with a large national chain. Other
hospital-based
systems in central Phoenix are struggling to maintain market share,
and some have moved to position themselves in the
suburbs. Physicians are seeking new ways to organize and shore up
their declining incomes, with an emerging emphasis
on single-specialty networks and joint ventures. Bolstered by new
tobacco tax dollars, the safety net for the uninsured
in Phoenix remains in place, but the uncertain future of the county-owned
system is a cause for significant concern.
uring the past two years, national
for-profit managed care companies have solidified their hold on Phoenix’s health
plan market. The largest local hospital system has undergone dramatic
reconfiguration and has aligned with a large national chain. Other
hospital-based
systems in central Phoenix are struggling to maintain market share,
and some have moved to position themselves in the
suburbs. Physicians are seeking new ways to organize and shore up
their declining incomes, with an emerging emphasis
on single-specialty networks and joint ventures. Bolstered by new
tobacco tax dollars, the safety net for the uninsured
in Phoenix remains in place, but the uncertain future of the county-owned
system is a cause for significant concern.
As the Phoenix health care market continues to develop, the following issues merit particular attention:
- How will the Phoenix market be
affected by the growing influence of national chains in the hospital and health
plan sectors?
- What impact will the reconfiguration
of the hospital market have on competition among providers and the services
available to Phoenix residents?
- Will Medicare HMOs change their
benefit packages and institute premium-sharing requirements for enrollees,
in light of anticipated local changes
in the program?
- How will health care systems respond to new pressures from physicians for
entrepreneurial partnerships?
- What changes are in store for the safety net, given the uncertainty facing Maricopa Integrated Health System and the growing number of uninsured? Will tobacco tax dollars provide sufficient funding to serve the poor?
Phoenix Compared to Other Communities HSC Tracks
Phoenix, the highest and lowest HSC study sites and metropolitan areas with over 200,000 population
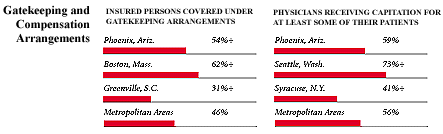
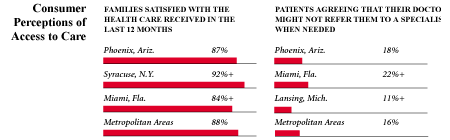

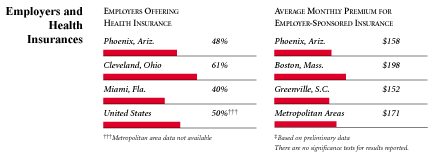
+ Site value is significantly different from the mean for metropolitan
areas over 200,000 population.
The information in these graphs comes from the Household, Physician and Employer
Surveys conducted in 1996 and 1997 as part of HSC’s Community Tracking Study. The
margins of error depend on the community and survey question and include +/- 2
percent to +/- 5 percent for the Household Survey, +/-3 percent to +/-9 percent
for the Physician Survey and +/-4 percent to +/-8 percent for the Employer Survey.
Background and Observations
Phoenix Demographics
| Phoenix, Ariz. | Metropolitan areas above 200,000 population |
| Population, 19971 | |
| 2,839,539 | |
| Population Change, 1990-19971 | |
| 26% | 6.7% |
| Median Income2 | |
| $24,911 | $26,646 |
| Persons Living in Poverty2 | |
| 15% | 15% |
| Persons Age 65 or Older2 | |
| 14% | 12% |
| Persons with No Health Insurance2 | |
| 16% | 14% |
|
Sources: 1. U.S. Census, 1997 2. Household Survey Community Tracking Study, 1996-1997 | |

The Community Tracking Study, the major effort of HSC, tracks changes in the health system in 60 sites that are representative of the nation. Every two years, HSC conducts surveys in all 60 communities and site visits in the following 12 communities:
- Boston, Mass.
- Cleveland, Ohio
- Greenville, S.C.
- Indianapolis, Ind.
- Lansing, Mich.
- Little Rock, Ark.
- Miami, Fla.
- Newark, N.J.
- Orange County, Calif.
- Phoenix, Ariz.
- Seattle, Wash.
- Syracuse, N.Y.